Urinary tract infections after menopause are more common than many women expect. For some, a UTI appears after decades without one. For others, infections begin to recur, creating frustration and uncertainty.
New research is helping explain why this shift happens. Scientists are learning that postmenopausal UTI risk is closely tied to changes in estrogen levels, tissue strength, and the vaginal microbiome—especially the loss of protective Lactobacillus bacteria that help maintain the body’s natural barrier against infection.
Understanding these changes reframes the conversation from treatment alone to prevention.
The Body’s Natural Protective Barrier
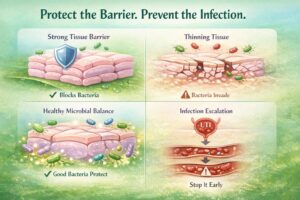
The tissues lining the vaginal and urinary tract form a natural barrier that helps block bacteria from entering deeper layers. Living alongside those tissues are beneficial bacteria—particularly Lactobacillus—that maintain an acidic environment where harmful microbes struggle to grow.
Together, these tissues and protective bacteria function like a shield.
During reproductive years, estrogen—specifically 17-beta estradiol—helps keep these tissues thick, resilient, and well-nourished. It also supports the growth of Lactobacillus, reinforcing the body’s microbial balance.
What Changes After Menopause
After menopause, estrogen levels decline. As this happens:
- The epithelial lining of the vaginal and urinary tract can become thinner and more fragile.
- Lactobacillus dominance in the vaginal microbiome often decreases.
- The environment becomes less acidic and more permissive to potentially harmful bacteria.
When tissue resilience and microbial balance shift at the same time, natural defenses weaken. This is one reason urinary tract infections become more common in midlife.
A recent scientific review in Frontiers in Microbiology highlights how menopause reshapes microbial ecosystems across multiple body sites—particularly the gut, vaginal tissues, and urinary tract. These systems interact with one another and with the immune system, meaning changes in one area can influence vulnerability in another.
Why Prevention Matters
Most urinary tract infections are treatable when recognized early. However, when untreated or unrecognized, bacteria can travel upward into the kidneys. In rare cases, infection can enter the bloodstream and lead to urosepsis, a serious systemic condition.
Because of this risk, researchers and clinicians are increasingly focused on prevention rather than reaction.
Protecting the body’s natural barrier—supporting tissue health and maintaining microbial balance—reduces the likelihood that infection begins in the first place.
Local replacement of 17-beta estradiol in the vaginal tissues is one strategy clinicians may consider to help maintain tissue resilience and support protective microbial conditions. Women experiencing recurrent urinary tract infections after menopause may wish to discuss this option with their healthcare provider.
A Prevention Mindset
At My28Days®, we sometimes describe this goal as Zero UTI—not as a guarantee that infections will never occur, but as a prevention-oriented mindset.
Healthy tissues.
Healthy microbial balance.
Early attention to symptoms.
These principles support resilience.
As research on the microbiome and hormonal health continues to evolve, one message becomes clear: the body was designed with strong defenses. When those defenses are supported, they often function remarkably well.
Conclusion
Urinary tract infections after menopause are not random. They reflect understandable biological shifts in estrogen levels, tissue integrity, and microbial balance.
When we understand how the body protects itself, we can work with it—strengthening the natural barriers that prevent infection before it begins.
Protect the barrier.
Prevent the infection.
When we understand how the body protects itself, we can work with it—supporting the quiet systems that help keep us well.
Read the full study at Frontiers:
My28Days.org is an educational and advocacy platform supported by the Mary Elizabeth Conover Foundation. For more information or to lend support, contact Office@ConoverFoundation.org




